The Cost of Waiting
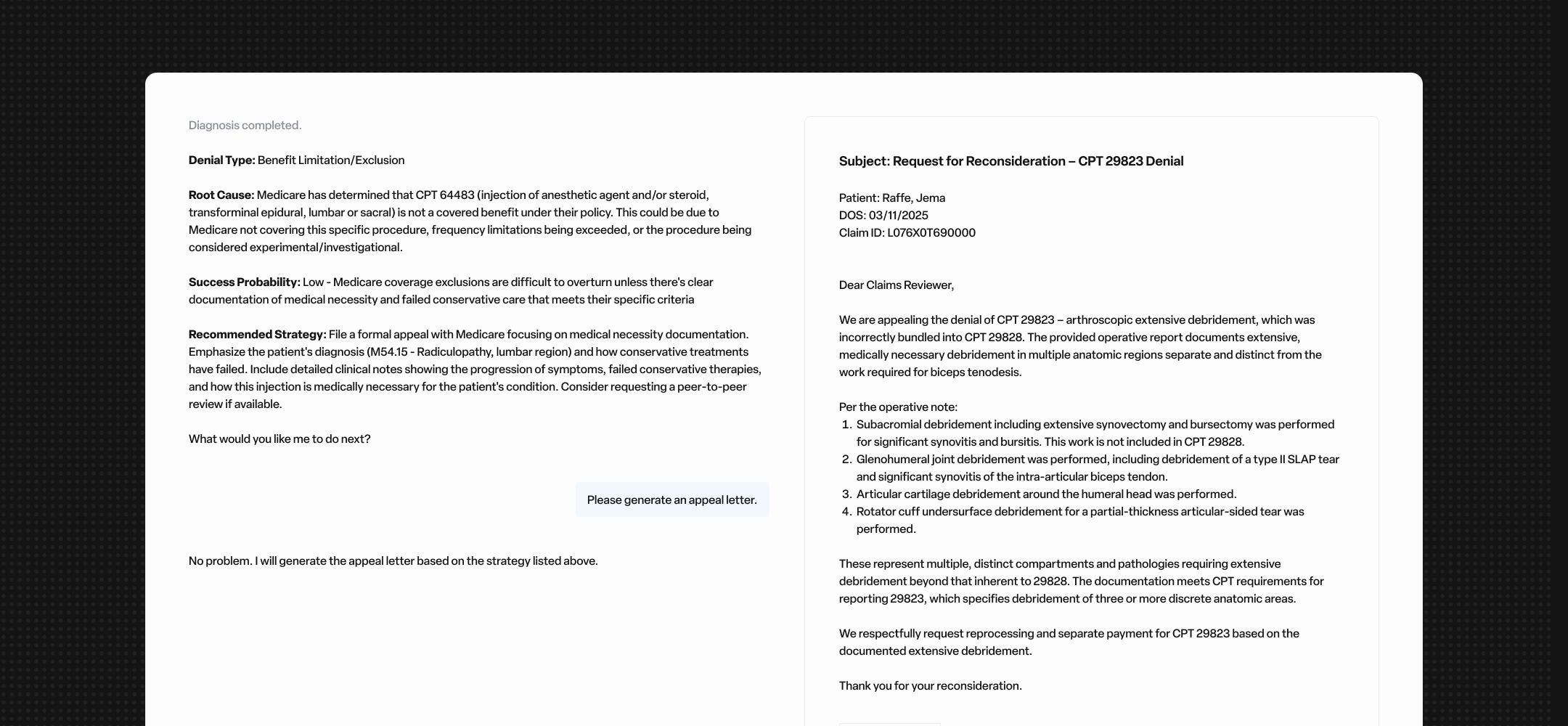
Denials are rising, but denial teams are not growing with them. Staff resolve each case one at a time, reading clinical documentation and determining the right path forward. Appeal letters are manual, inconsistent, and slow.
No one has time to step back and analyze what is driving the volume. Gaps in coding, documentation, or payer behavior go unnoticed until they show up in a quarterly report, after the revenue has already been lost.